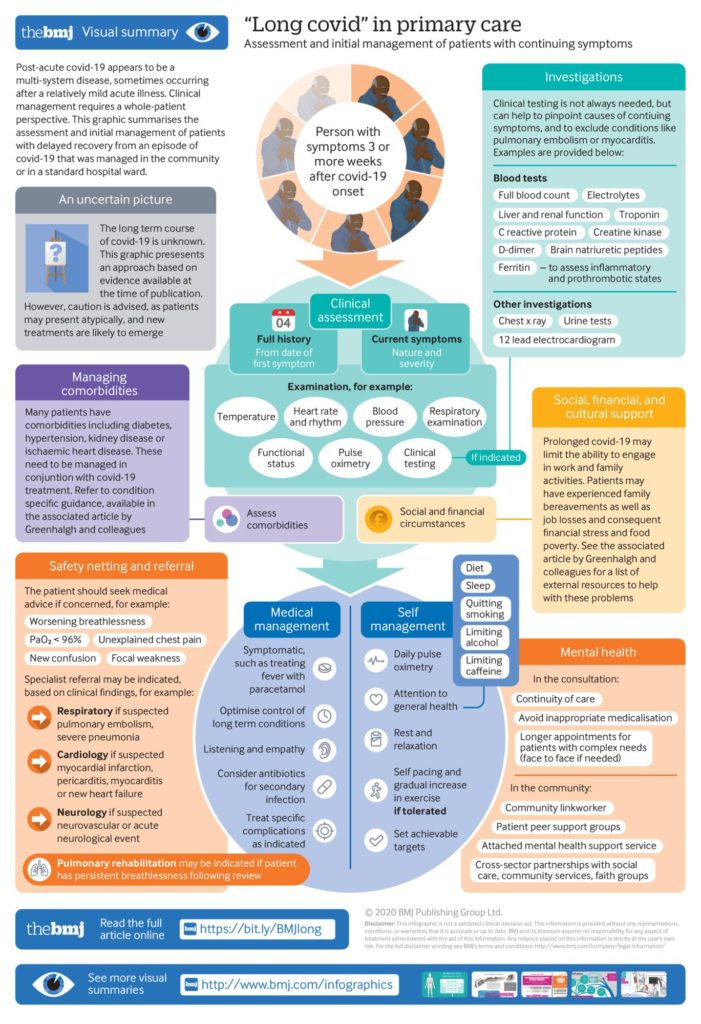
The NHS will have to hire more than 1,000 new consultants, physios and counsellors to treat patients with the lingering and sometimes life-threatening ‘side effects’ of COVID-19, a new report presented by Trisha Greenhalgh, Professor of Primary Care Health Sciences University of Oxford, to the House of Lords select committee has indicated.
Long Covid is a distinct condition affecting approximately 60,000 people in the UK and is characterised by persistent and fluctuating fatigue.
Other signs of concern include breathlessness, cognitive blunting (“brain fog”) and pain. The cause is unknown but it is likely to be due at least partly to an inflammatory reaction. Many cases remain undiagnosed, since some clinicians may incorrectly require a positive test for Covid-19.
But for some, such as British author Michael Rosen, who was placed into an induced coma in March and is still suffering from symptoms including sight and hearing loss, attests that COVID has taken many ‘victims’. Please listen to his account in the BBC news segment via the video above.
Call for more care
Greenhalgh says those suffering long-term effects were experiencing “inconsistent and fragmented care” and recommended urgent action. As part of the written evidence, she and her fellow researchers suggested a four-tier clinical service was required, comprising self-care, generalist care, specialist care and specialist management of specific complications.
Greenhalgh and Dr Emma Ladds of University of Oxford; Dr Matthew Knight, Watford General Hospital; and Dr Deepak Ravindran, Royal Berkshire Hospital have suggested as part of their study that approximately 60,000 people in the UK probably have long Covid, which based on these figures as implications for GP practices.
For example, a GP practice with 20,000 patients in an area of high Covid-19
incidence (e.g. London, Leicester) is likely to have:
- Up to 2000 patients who have had Covid-19 (whether test-confirmed or
not) - Up to 200 patients whose Covid-19 required a sick note for more than 3
weeks. - Up to 100 patients with some form of chronic Covid-19 (i.e. not completely better by 12 weeks).
- 10-20 patients with seriously debilitating chronic Covid-19 (e.g. unable to
work or take part in normal family life or leisure activities).
Long Covid services are currently “patchy and overstretched”, according to Greenhalgh. This is partly because funding was diverted away from rehabilitation and towards the acute sector as an emergency response to the pandemic.
Specialist rehabilitation services designed for patients recovering from a hospital admission (e.g. oriented to restoring normal breathing after pneumonia) have become swamped with referrals from general practice (who often have more general symptoms such as fatigue).
NHS-linked recruitment agencies will therefore be wise to start scouting out candidates now as the number of COVID patients in hospital rises and the anticipated roll-over of Long COVID complications follow, just as the country also heads into Flu season.